Advocates say the fix for Virginia’s broken mental health care system isn’t necessarily more beds
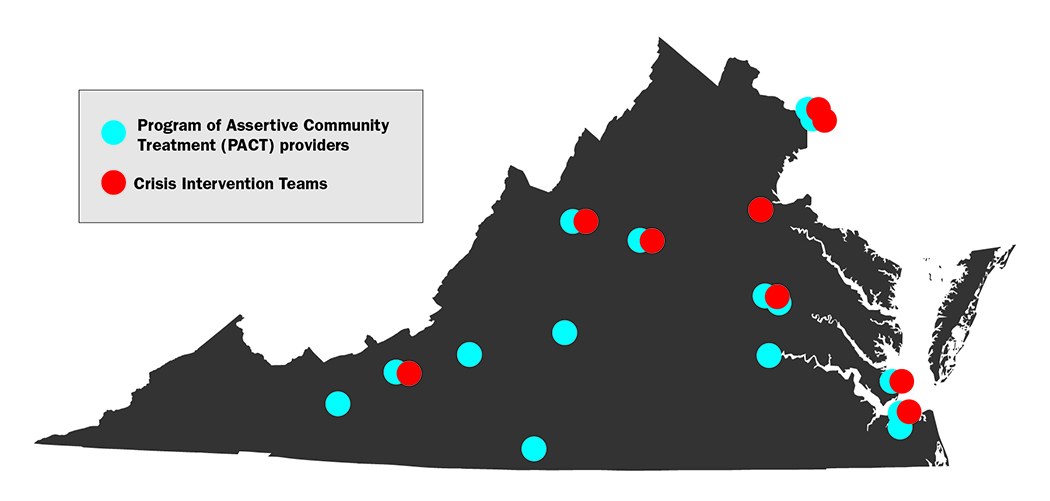
Mapping mental health care: Governor McDonnell’s proposed budget expansion includes millions over the course of two years for two highly regarded community-based mental health care programs: Crisis Intervention Teams, which consist of police officers trained to defuse mental health crises and steer patients to the care they need, and Program of Assertive Community Treatment, or PACTs, outpatient care networks designed to keep the severely mentally ill out of hospitals.
Large swaths of Virginia lack access to either program, but the Charlottesville area is among the regions in Virginia with both—and advocates say building up such programs is the best way to keep people healthy and help them avoid costly, restrictive hospital stays.
Support C-VILLE Weekly
C-VILLE Weekly is Charlottesville’s leading newspaper. Founded in 1989, it’s been the area’s local source for informative (and informed) stories in news, arts, and living for more than 26 years.
UP NEXT
In brief
The Big Picture
Hall pass
Songs and stories
IN CASE YOU MISSED IT
In brief
The Big Picture
Hall pass
Songs and stories
PUBLICATIONS
C-VILLE Weekly | April 24, 2024
C-VILLE Weekly | April 17, 2024
C-VILLE Weekly | April 10, 2024
C-VILLE Weekly | April 3, 2024
Real Estate Weekly | April 24, 2024
Real Estate Weekly | April 17, 2024
Real Estate Weekly | April 10, 2024
Real Estate Weekly | April 3, 2024
Abode | Spring 2024
Knife & Fork | Spring/Summer 2024
Fine Properties | Spring 2024
Weddings | Fall/Winter 2023
Best of C-VILLE 2023
We Are C-VILLE | March 2024
Summer Camp Guide | March 2024
National Nonprofit Day | August