UVA study testing ultrasound surgery treatment on Parkinson’s patients
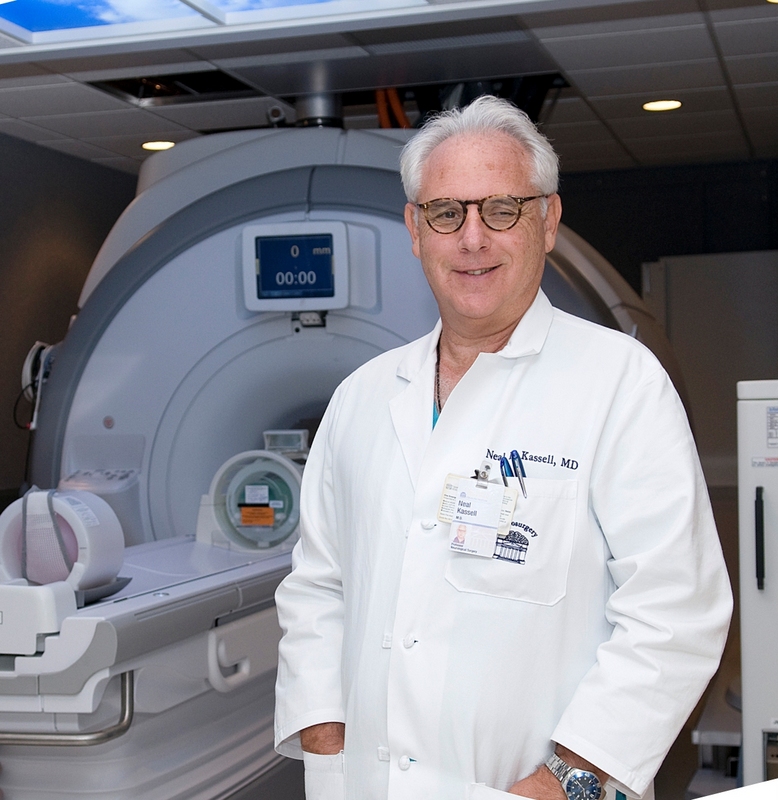
UVA neurosurgeon Neal Kassell has given up the OR in favor of working to advance a surgical technology he says could be the most important medical device development since the invention of the scalpel—and he’s building a new research funding model in the process. Photo courtesy of UVA Medical Center.
Support C-VILLE Weekly
C-VILLE Weekly is Charlottesville’s leading newspaper. Founded in 1989, it’s been the area’s local source for informative (and informed) stories in news, arts, and living for more than 26 years.
UP NEXT
Sweet spring tradition
Tiptoe thrills
Mountain mindful
Murder farm
IN CASE YOU MISSED IT
Sweet spring tradition
Tiptoe thrills
Mountain mindful
Murder farm
PUBLICATIONS
C-VILLE Weekly | April 10, 2024
C-VILLE Weekly | April 3, 2024
C-VILLE Weekly | March 27, 2024
C-VILLE Weekly | March 20, 2024
Real Estate Weekly | April 10, 2024
Real Estate Weekly | April 3, 2024
Real Estate Weekly | March 27, 2024
Real Estate Weekly | March 20, 2024
Knife & Fork | Spring/Summer 2024
Fine Properties | Spring 2024
Abode | Winter 2024
Weddings | Fall/Winter 2023
Best of C-VILLE 2023
We Are C-VILLE | March 2024
Summer Camp Guide | March 2024
National Nonprofit Day | August